Hip Procedures / Resurfacing Arthroplasty |
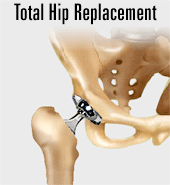
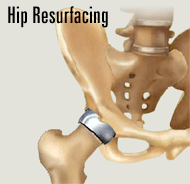
The hip joint is a ball and socket joint where ball of the thigh bone (femur) joins with the socket (acetabulum) of the pelvic bone. The ball is normally held in the socket by very powerful ligaments that form a complete sleeve around the joint (the joint capsule). The capsule has a delicate lining (the synovium). The ball is covered with a layer of smooth cartilage which is a fairly soft, white substance. The socket is also lined with cartilage. This cartilage cushions the joint, and allows the bones to move on each other with very little friction. An x-ray of the hip joint usually shows a "space" between the ball and the socket, which in reality is the gristle (cartilage) because, the cartilage does not show up on x-rays. In the normal hip this "joint space" is approximately 5mm wide and fairly even in outline. This joint space, on the x-ray, reduces significantly when the hip joint is diseased, most commonly due to arthritis (osteoarthritis). Other conditions, such as avascular necrosis also may lead to breakdown of the hip joint. Resurfacing arthroplasty of the hip is a surgical procedure in which the surgeon replaces only joint surfaces of the ball (head of the femur) and the socket (acetabulum) with new, artificial parts, called prostheses. The procedure usually lasts 60 to 90 minutes. The new hip is based on metal-on-metal bearing that is meant to allow a natural, gliding motion of the joint due to fluid film lubrication. The goals of resurfacing arthroplasty are to improve the quality of life in young active patients where a total hip replacement may be an over kill. |
||
 |
 |
|
| Usually, people do not spend more than 5-7 days in the hospital after resurfacing arthroplasty of the hip. Full recovery from the surgery takes 2 to 3 months, some times more, depending on the type of surgery, the overall health of the patient, and the success of rehabilitation. | ||
What to expect as a patient of HIP RESURFACING |
You are examined by me and, if suitable, a decision to proceed with resurfacing surgery is made. This is a co-operative decision between you, me, your family and your local doctor. The whys and wherefores of this surgery are discussed in detail with you. Main benefits to be expected of this surgery are |
• |
Less bone resection
|
• |
Reduced hip pain
|
• |
Improved quality of life, ability to return to normal activities. |
• |
Return to sports such as tennis, golf, bowls, cycling, and long walking. It is not advisable to be running following a resurfacing arthroplasty. |
| Pre-operation | |
• |
You will be sent for routine blood tests and any other investigations required prior to your surgery a week before surgery. |
• |
You will be asked to undertake a general medical check-up with a physician when necessary. |
• |
You should have any other medical, surgical or dental problems attended to prior to your surgery. |
• |
Stop smoking as long as possible prior to surgery. |
| Day of Surgery | |
• |
You will be admitted to hospital usually day before or on the day of your surgery. |
• |
Further tests may be required on admission. |
• |
You will meet the nurses and answer some questions for the hospital records. |
• |
The anaesthetist will discuss with you the type of anaesthetic. Anaesthesia may be either general or regional. |
• |
Usually the anaesthetist will either sedate you or give you a full anaesthetic if you have a spinal/epidural procedure. |
• |
You will be given hospital clothes to change into. |
• |
Approximately 30 minutes prior to surgery, you will be transferred to the operating theatre. |
Surgery |
Surgery essentially involves exposure of the diseased ball and socket joint and replacing both joint surfaces with man-made, artificial metal-on-metal bearing surfaces. Contrary to the belief, the scar is usually much bigger, than a total hip replacement scar, after a resurfacing arthroplasty. In the recent years, uncemented components have shown very impressive results and, as a result, I prefer to do uncemented resurfacing for both ball and socket components. Following insertion of the components the wound is closed usually with absorbable sutures inside and a drain is inserted. Skin usually gets removable sutures. |
Post Operation |
You will wake up in the recovery room with a number of monitors to record your vital signs such as blood pressure, pulse, oxygen saturation and temperature. You will have a dressing on your hip and a drain coming out of your wound. Post-operative x-rays will be performed in recovery. Once you are stable and awake you will be taken back to the ward. You will have one or two drips in your arm for fluid and pain relief. This will be explained to you by your anaesthetist. On the same day, or occasionally, day following surgery, your drains will be removed and you will be allowed to sit out of bed or walk under the supervision of a physiotherapist. You will be able to put all your weight on your hip, unless conditions dictate otherwise, and your physiotherapist will help you with the post-op hip exercises. You may experience some pain and discomforts, which will be kept under control with medications, but if you are in a lot of pain, inform your nurse. Based on my training and experience from a high volume hip surgery unit in Cambridge, England, I am persuaded to believe that patients may be permitted to mobilise as soon as they can, as the hip allows them to do so. There are really no major restrictions on mobilisation and, it is important to mobilise as soon as you are comfortable as this will prevent complications such as deep vein thrombosis and chest infections. You will be discharged to go home approximately 3-5 days sometimes longer, depending on your mobility and help at home. Sutures are usually removed at two weeks. |
Risks and complications after resurfacing arthroplasty of the hip: |
|||||||||||||||||||||||||||||||||||||||||||||
|
General advice after resufacing arthroplasty |
You should have a regular check every year with an x-ray. We do not yet have long-term results although, short and medium-term results are good. If you have had any major bowel, bladder or dental surgery, antibiotic cover should be given prior to the surgery. Metal prostheses can activate security alarms at the airports. |
Home | Know your Surgeon | Hip Procedures | Knee Procedures | Publications | Lectures | Gallery | Platelet - Rich Plasma Therapy | Contact us
